Novel Biomarker for Peridontal Disease
University of Pittsburgh researchers have identified a novel biomarker in saliva samples, sTREM2 protein, to detect the presence of periodontal disease (PD) or periimplantitis. Using this biomarker, clinicians could determine if a patient is suitable for a dental implant and inform treatment decisions for patients with PD. Development, validation, and clinical use of this biomarker could improve outcomes in patients with PD or periimplantitis, reduce damage to gums and surrounding tissue including the alveolar bone, and prevent tooth loss.
Description
Periodontal disease, infection of the gums and bones in the mouth, affects approximately 45% of Americans at some point. Disease onset can be delayed following initial infection with untreated disease resulting in tooth loss and other irreversible damage to the periodontal tissue. Current treatment strategies can be suboptimal – there is a clinical need to develop methods of detecting infection before the onset of severe disease symptoms, to allow for early treatment and reduce the risk of long-term tissue damage. Identifying patients with periimplantitis earlier can aid clinicians in decision-making prior to any dental implantation surgery (e.g., crown or bridge) to reduce the risk of implant failure.Applications
- Periodontal disease screening- Presurgical screening for orthodontic patients
Advantages
The triggering receptor expressed on myeloid cells 2 (TREM2) is a transmembrane receptor with an immunoregulatory role. Previous work has demonstrated that levels of soluble TREM2 (sTREM2), produced during times of infection, can be detected in serum, plasma, and cerebrospinal fluid and can be used as a biomarker of infection. However, detection of sTREM2 in saliva had not previously been achieved.This novel approach uses saliva samples to detect the presence of PD based on level of sTREM2 and other markers of inflammation. This non-invasive approach is particularly advantageous to patients and clinicians allowing for earlier diagnosis of PD. This novel biomarker could result in lateral flow devices or other real-time diagnostic methods being developed improving access to diagnosis tools and early diagnosis of PD in low-resource or human and animal healthcare.
Invention Readiness
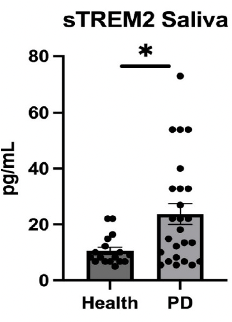
Saliva samples from healthy (n=20) and diagnosed patients with PD (n=26) were analysed. Significantly higher levels of salivary sTREM2 were observed in patients with PD. More severe PD was associated with higher salivary levels of sTREM2. Further optimisation and validation are required and sTREM2 has the potential to be a clinical useful biomarker for PD.IP Status
Patent PendingRelated Publication(s)
Leite, T. C., Chen, J., Diacou, A. A., Park, S., Jheon, A. H., Yin, J., Easter, Q. T., Fitz, N. F., Byrd, K. M., & Clark, D. R. (2025). Macrophage dynamics and the role of TREM2 at the oral mucosal barrier. Journal of translational medicine, 23(1), 1135. https://doi.org/10.1186/s12967-025-07135-5
Clark, D., Brazina, S., Miclau, T., Park, S., Hsieh, C. L., Nakamura, M., & Marcucio, R. (2024). Age-related changes to macrophage subpopulations and TREM2 dysregulation characterize attenuated fracture healing in old mice. Aging cell, 23(9), e14212. https://doi.org/10.1111/acel.14212
